'Surges of new variants for the foreseeable future,' amid progress, says a leading COVID-19 expert
Q&A with Dr. Jeremy Faust, author of "Inside Medicine," a Bulletin newsletter, who discusses a 'COVID-weary' nation, what you should know about Paxlovid, BA.5, mental health and the pandemic's future.

Editor's note: Black Iowa News interviewed Dr. Jeremy Faust, who writes 'Inside Medicine" on Bulletin. The COVID-19 expert answered seven important questions about the state of the coronavirus pandemic. Faust is an emergency medicine physician at Brigham and Women's Hospital in Boston, Massachusetts, and an instructor at Harvard Medical School. He is also the editor-in-chief at MedPage Today.
Subscribe to Black Iowa News. Thanks for reading.
 |
While the Omicron subvariant BA.5 sweeps the nation, many Americans are apathetic and weary about the future of the coronavirus pandemic — and they're at increased risk of infection or reinfection. Back-to-school time looms, along with new face mask mandates in some places. But one of the nation's leading COVID-19 voices, Dr. Jeremy Faust, doesn't want Americans to get "discouraged." He answered seven questions from Black Iowa News about the state of the nation's mental health, the antiviral #Paxlovid, back to school, COVID-19 vaccines and testing, Omicron subvariant transmission and our pandemic "new normal."

Dr. Jeremy Faust writes Inside Medicine on Bulletin. Faust is an emergency medicine physician at Brigham and Women's Hospital in Boston, Massachusetts, and an instructor at Harvard Medical School. He is the editor-in-chief at MedPage Today. Photo courtesy of Faust. |
Black Iowa News: How is the protracted coronavirus pandemic affecting our overall mental health and what should we do if we're experiencing anxiety and depression?
Dr. Jeremy Faust: "We are all just tired, and I think that there are two angles to the mental health fatigue and the first is that the virus itself is just so much to deal with. Because people know someone who has been affected. They know someone who has died, who has been hospitalized. Or they themselves have had an illness that was unexpectedly burdensome. Or their symptoms lasted longer than they thought they would. Or they have Long Covid. So when we talk about mental health and the pandemic, a lot of times it's sort of a dog whistle for people saying we've overreacted and like it's the shutdown that made people kind of lose their mental sort of stability, or it's the lack of connectivity. I think there's some of that, but I also think that so much of it is just the fatigue — the emotional and mental fatigue — of living in the presence of a virus that can really harm lives, and obviously it hit seniors the worst, but young people can also have bad outcomes.
So I think that there is just this menace that is with us, and as a result, we are collectively tired, which is some of the reasons why we're not doing as much, right? That's why we're not masking as much. It's why we're not willing to change our behavior when there's surges, and that's too bad, because we've got lives to live, and we need to live them. I fear it's going to get worse. So that's very depressing, isn't it?

|
What should we do if we're experiencing anxiety and depression? Well, first of all, I actually think that one positive thing that's come out of the pandemic, for those with means anyhow, is that telehealth is a lot easier. Like finding help online with mental health, psychiatrists, psychologists, counselors, it's just easier to find people because the people who provide these services for now are willing and able to do it via telehealth. So you don't have to kind of like reorganize your entire day or week even to get those services, but obviously, that's really dependent on the ability to use those services, and it's not a given for all people. So for me, it might be easy to get a psychiatrist, but it might not be for everybody. So the good thing is these resources are out there and they can be very helpful.
At the extreme end, we also have a new tool which is calling 988. We used to have 911, only now we have 988, the national hotline for mental health crises. And people are calling on a suicide hotline, and it is that, but it's not just that, and I think that it's a place to start for people who really don't know where to turn. Boy, it's a lot. But I think that the bright side is that there are some more resources than there used to be. And it's important that we not stigmatize using them. So let's use them, and you know, if I do, I'm going to brag about it. I'm not going to hide it."
Black Iowa News: Some people with current COVID-19 infections have sought out Pfizer's COVID-19 antiviral, Paxlovid, which is trending on Twitter. How does it work in the body, how likely is someone to experience "Paxlovid rebound" and what should at-risk patients do if their doctors/pharmacists refuse to prescribe it?
Dr. Jeremy Faust: "Paxlovid is an antiviral medication. It actually stops the virus from replicating. And that seems like a really good idea. Lots of medications do that. But this is the one that seems to actually do so in a way that really decreases the likelihood of severe illness or hospitalization. And it was studied in unvaccinated people, and it had a major effect. With vaccinated people, it looks like the data are less clear on this, but from what we can tell, it seems to help some vaccinated people, as well as especially older vaccinated people or people with a lot of risk factors. I don't think the young and healthy need it. I am not really that young. I am 43, and I'm pretty healthy. If and when I get COVID, I do not expect that I will be taking Paxlovid, but I don't think I need it. I have a little bit of asthma, but I'm not worried that that's going to make me go to the hospital.
So I'm actually seeing two things: I'm seeing it under-prescribed in at-risk patients, and I'm seeing it over-prescribed in the young, healthy and wealthy. But how do we get it to people who need it? But I actually think that, you know, basically push back. Because if you're an older person or a person with risk factors, or especially an unvaccinated person, but even if you're vaccinated and have real risk factors, I think that the doctors and pharmacists need to just be given a second chance to hear that again, that may not solve it, but say 'Look, the CDC says that at-risk patients like me should get Paxlovid. Why would I not get it?' And they might have a good reason like, 'Oh, it's been too long, or it interacts with medication you're taking.' But I think that we should feel emboldened to push back on the people who are saying no, in the cases where the answer should be yes."

Source: Canva |
Black Iowa News: Back-to-school time is around the corner. What are the benefits/risks of vaccinating young children against COVID-19?
Dr. Jeremy Faust: "I am very in favor of vaccinating young people, young children. Because even though COVID-19 is far less likely to cause a terrible outcome in toddlers and babies and kids, the truth is that it's not harmless to get COVID for these kids, and there are hospitalizations, there are deaths, and we have no idea about other long-term consequences. We just don't know. We do know these vaccines are safe. We do know that it eliminates the hospitalization basically, for some people, early in the pandemic, and even with the new variants, they're still very effective. So I think that the best way, for me as a parent, to have peace of mind knowing that my kid can go and do the things that I want them to do as kids, the way I'm getting that peace of mind, is by vaccinating my kids, so that if and when they do get infected, it will basically be mild. I think it's huge, and I'm really hoping that parents will look at back to school as a little nudge to do it . . . But we need to do it because the rates have been low and it's a population that we want to protect. It's super safe."
Black Iowa News: Does testing positive for COVID-19 mean an individual is contagious until the point that they test negative (even if that takes weeks?) (Should people isolate until such time that they test negative?)
Dr. Jeremy Faust: "So there are two kinds of tests that, broadly speaking, there are PCR tests, which check for the genetic material of the virus, and those are generally tests that you would get at like a pharmacy drive thru or at the doctor.
And then there's these at-home rapid antigen tests and that checks to see if in your nose there is actually like the surface of the virus, like the proteins that make up the surface of the virus.
And so, the PCR test, the genetic tests are much more sensitive, they become positive sooner and they stay positive longer. And that's great for diagnosing, but the problem is that if you were to go back to that pharmacy and recheck in a week or two, you might still be positive on that PCR, but that does not mean you're still contagious.
So the PCR, that genetic test, just means you're infected, or you have been infected recently, versus the at-home rapid antigen tests . . . These, as I mentioned, they check for actual proteins that make the surface of the virus up and tell you whether or not you actually have a lot of virus . . . in your nose. Those should become negative within basically 10 days.

Young woman undergoing a COVID-19 test. Source: Getty Images. |
People who take Paxlovid, they might have this rebound where they become positive on those rapid tests again, and basically if you are positive on a rapid at-home test, you should be considered contagious. If those rapid at-home tests are showing those lines on the test line that says you're positive, you've got to consider yourself contagious. Paxlovid rebound is when someone who gets infected with coronavirus takes Paxlovid but then their symptoms get a little better. They might start to test negative on an at-home rapid antigen test, and then they have this rebound where they start to feel worse again and they check to see if they've tested positive again, and lo and behold, it is.
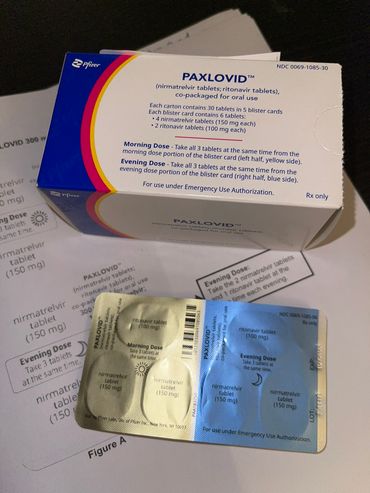
Pfizer's Paxlovid antiviral is intended for at-risk patients with COVID-19. It is used within the first five days of testing positive for COVID-19 and can be prescribed by doctors and pharmacists. Photo by Black Iowa News. |
So it's this idea that you go from positive to negative back to positive again, and your symptoms go from not feeling great to feeling better to feeling worse again. And Paxlovid is causing this, we don't know how common it is. I think it is more common than the 1% or so that they picked up in the clinical trials. I don't know whether it's 5%, 10%, 20%, but it's certainly a lot higher than we initially thought. And it's a reason for young healthy people not to take Paxlovid, if you ask me. You'd like this thing to be over in 10-12 days, not 15 or 20.
But long story short on the testing, your PCR genetic test is going to stay positive for a long time, it does not mean you are contagious for weeks and weeks. Whereas the rapid antigen at-home test should not stay positive after 10-12-14 days . . . But as long as you're testing positive on a rapid antigen, you are contagious, and you need to isolate."
|
Twitter
See @polkcohealth's post on Twitter.
twitter.com/polkcohealth
|
|
Black Iowa News: It's summer. With the rise of highly contagious Omicron subvariant BA.5, how safe are we outdoors and which outdoor activities, if any, should we avoid?
Dr. Jeremy Faust: "Outdoor is the safest. We're never going to get to zero risk. It's impossible. And everything is sort of on a spectrum. If you're indoors with someone for two seconds, and you didn't have mask on, but then you realize that your risk is low. Even though you're indoors with someone who was like spouting out Omicron particles into the air. Whereas if you're outdoors and you're at a rock concert and you're screaming in the faces of your neighbor for five hours just over and over again and you're just like shouting particles of Omicron into their face. You know, eventually it's going to get in there. So even though it's outdoors, everything's on a spectrum.

Couple walking outdoors. Source: Getty Images. |
So outdoors generally is much safer, and indoors is less safe, but if you do indoors correctly, it's safe, and if you do outdoors incorrectly, it's unsafe . . . We're not going to lock down for the rest of our lives. We're not going to not do stuff. So I have a pretty liberal attitude towards outdoors. But when we took our four-year-old to a street fair and it was really, really crowded, I was like: Let's just kind of avoid the really, really crowded part. But probably even that's overkill because, again, outdoors is so safe. But again, there's going to be exceptions, and I don't want anyone to misunderstand: Like you can get it anywhere, anytime. It's just the outdoors is so much safer. I don't even make my kids, the one who was old enough, wear a mask outdoors, except in extreme circumstances. Whereas indoors, she still wears a mask when she goes to preschool and all that kind of stuff."
|
Twitter
See @jeremyfaust's post on Twitter.
twitter.com/jeremyfaust
|
|
Black Iowa News: Where is the most reliable source of COVID-19 data for the public?
Dr. Jeremy Faust: "Well, they can read my fancy newsletter: Inside Medicine. The CDC data is actually reliable, it's just hard to navigate and find everything. There are some really good social media accounts. One problem that I'm having with Twitter, which I love. I do love Twitter — is that there is a little bit of alarmism — like 'every new variant is the worst ever. We're back to square one.' It's like — No, we're not. It's not good, but we're not that bad. The vaccines still work, and we can test for it now. And, of course, on Twitter, you also see people being like 'Oh, coronavirus, it's like a cold. It's nothing.' That's obviously downplaying and terrible. I get a lot of good information from social media, but I know how to curate it. That's what I kind of do.
"It's so hard to say there's good stuff on social media, because there is, and there's also terrible stuff on social media."
. . . State and local departments of health have done a very, very good job. So actually, that's a great resource. There are some good blogs out there like mine. There's an epidemiologist named Katelyn Jetelina. She has a Substack, which is really, really good."
Black Iowa News: It has been two and a half tumultuous years. Is this the new normal? Endless virus surges and waves, face masks and booster shots?
Dr. Jeremy Faust: "Oh my gosh, I hope not. I don't think so. I think that some things are never going to go back, and that's a good thing. So I think that like when we have surges of any virus, we should be testing people for them, for contagiousness and using rapid tests to see if they should go to school or not, whether it's coronavirus, Influenza, RSV, we should be testing people for viruses that can kill people if we spread them to the wrong folks. So that's a new normal that I think is a good thing.
"Like let's stop pretending viruses just affect everyone mildly and the same and equitably and sort of evenly distributed. It's like not true. So let's use the tools we've learned to use during this pandemic."
For now, I think we're going to have surges of new variants for the foreseeable future, which will mean keeping these tools in our pockets, or on our faces, as needed. And obviously people have different levels of risk tolerance and people with different risk thresholds will respond differently each time. But I think for the foreseeable future, yes, it's going to be one wave after another.
But the meaning of those waves has changed, and this is why I want to make sure that people don't get discouraged. It's bad that BA.5 is here and is causing cases and hospitalizations. But it's not like really 2020, where every single patient that I treat has terrible pneumonia and is starving for oxygen and is going to be on a ventilator.
So we're making progress. I don't think that we have maxed out the progress. I think that we'll get better therapeutics, things that are better than #Paxlovid. It really decreases the risk of a very bad outcome like hospitalization, but it doesn't actually decrease how long you're sick and might even increase it. It doesn't render the virus sort of a non-issue, but I think we might get therapeutics that actually do sort of turn this virus into like essentially a meaningless or less important event than it currently is.
Man holding rapid antigen test. Source: Getty Images. |
I think that our vaccines are going to get better. We're going to have vaccines this fall that are targeted at Omicron and that's a good thing. I don't know how much it'll help. I think it will help some. I think we're going to have vaccines down the road that are better at just really addressing infection, like our vaccines do decrease infection temporarily, but they're really good just stopping severe disease, hospitalization and death. And I think that vaccines like nasal vaccines called mucosal vaccines might be like the sort of key to this all — in terms of making it so we can really stop the virus from being around us all the time.
We've made so much progress, and so right now we sort of have reached a little bit of a plateau in terms of these are the tools we have, let's use them, and we're not — we're not using them equitably, they're not being distributed equitably. So that's where we can make improvements. But then in the future, I think we'll also have new tools, and I think those tools will make it so that this current cycle of like new variant and question marks will become less frequent and less meaningful."
Subscribe to Inside Medicine
The latest on the Omicron subvariants: Data snapshot: The BA.4 and BA.5 Omicron variants. Where do things stand?
Subscribe to Black Iowa News
'COVID-19 is not going away' says Polk County Health official
Top Banner: Getty Images.

Become a subscriber. |



